Barry's Story
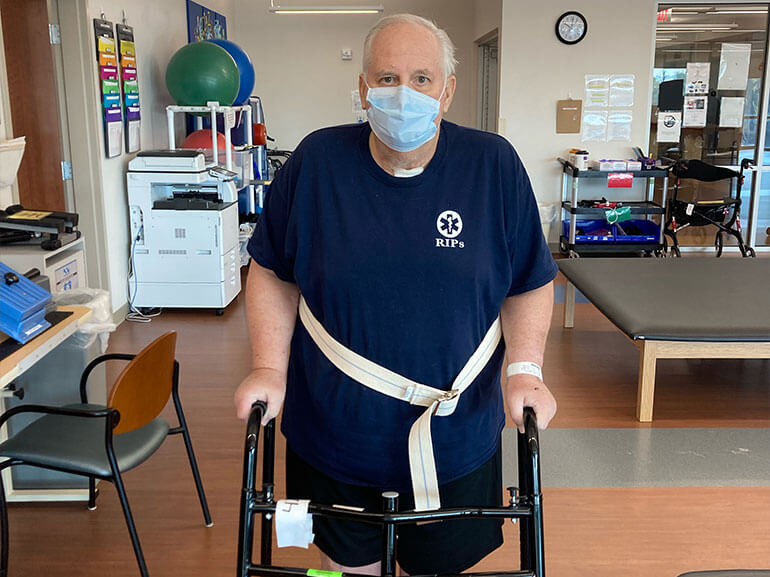
Barry Minnich, 68, is a fire chief in Luling, Louisiana who loves spending time with family. He has known his wife, Ann, since seventh grade, and they have four daughters and seven grandchildren. A couple days after knee replacement surgery, Barry noticed he was retaining fluid. He initially thought it might be from the procedure, but he was also having trouble breathing so he went to his primary care physician who performed a chest x-ray and lab work.
Test results revealed he was in heart failure and he was immediately sent to the local Emergency Department. He had surgery to clear blocked arteries in his heart, but there were many complications, and he spent 33 days recovering in the hospital. During his time in the hospital, a tube inserted into his windpipe assisted his breathing and a tube inserted directly into his stomach delivered hydration, nutrition and medication. After Barry stabilized, he was transferred to Ochsner Rehabilitation Hospital to continue his recovery.
When Barry first arrived, he was evaluated by the physical therapy team. He required significant assistance from multiple staff members to get out of bed and into a wheelchair, and to stand from the wheelchair. In order to protect his surgical incision and ensure proper healing, Barry was unable to bear weight through either arm, which significantly limited his abilities.
Barry’s physical therapy team worked with him on strengthening therapies to increase endurance with standing and walking. At the time of discharge, he was able to transfer and walk more than 150 feet with supervision and climb stairs with minimal assistance.
In occupational therapy, Barry initially required significant assistance with bathing, dressing, toileting and mobility. He was unable to eat and still had a feeding tube. He also had sternal precautions which meant that he was unable to use his arms to push to sit up or sit down in order to protect the surgical incision in his chest. Therefore, Barry had to rely on his legs for transferring positions. Barry participated in intense occupational therapy which consisted of strength, endurance and balance training. His therapist also focused on teaching Barry techniques to increase his independence with dressing and bathing through the use of adaptive equipment. As his strength and coordination increased and he mastered using the adaptive equipment, Barry progressed to dressing and transferring positions independently.
When Barry arrived at Ochsner Rehabilitation Hospital, he was “NPO,” meaning no food, liquid, or medication could be taken by mouth. All nutrition, hydration and medication were administered through the feeding tube inserted directly into his stomach. Barry’s speech therapist scheduled an instrumental swallow evaluation, known as FEES which stands for Fiberoptic Endoscopic Evaluation of Swallowing. A tube with a camera on the end is inserted into the nasal passage to view the patient’s throat while he/she eats and drinks various consistencies. If food or liquid is seen entering the airway, the patient is at risk of developing an infection known as aspiration pneumonia. The assessment revealed that Barry’s swallowing function had significantly improved to the point where he could safely tolerate eating and drinking by mouth again.
Barry also had a tracheostomy tube to improve his breathing. A tracheostomy tube provides an air passage to facilitate breathing when the usual route is blocked or obstructed. In Barry’s case, his tracheostomy tube also included a speaking valve which allowed Barry to talk. As the strength and conditioning in his throat muscles progressed, Barry was able to successfully regulate breathing through his nose and mouth, and his tracheostomy tube was capped.
Having family support played a huge role in Barry’s recovery. His wife and children visited every day, which motivated him to keep working hard. Reflecting on his experience, Barry also expressed gratitude for his care team at Ochsner Rehabilitation Hospital, “The encouragement and skilled services I received from my therapy team were excellent and helped me achieve my goals.”
After three weeks in inpatient rehabilitation, Barry was discharged home with plans to continue his recovery through several weeks of home health services and outpatient cardiac rehabilitation. At the time of discharge, Barry exceeded his goal of simply wanting to walk again, as he was walking without a cane and driving. Following discharge, he reported that he is now independent in all areas of self-care and able to drive himself to therapy and the fire station.
Barry’s advice to others on a recovery journey: “Stay vigilant in the routine, trust in what the therapists tell you and don’t set unrealistic goals. There will be successes every day even if you don’t realize it at the time.”